Leadership Project
During my time as a nursing student at the USC College of Nursing I have been happy with the quality of my education and the opportunities provided to me. However, I believe there are areas within the program where improvement would elevate student learning and increase student satisfaction. For instance, Senior preceptorship. This is the clinical component of NURS435, the Senior Capstone Practicum. This is very different from previous clinical experiences because we are no longer in a group. Instead, we are placed with a nurse on their unit to work. By the end of the semester we should be fulfilling the entire role of that nurse.
Faculty have stated that job prospects do not depend on preceptorship. While this is true, this final clinical experience sets the foundation and basis for our future nursing career. This can either negatively or positively affect our view as future nurses. In addition, this final clinical experience can have significant impacts on student nurses’ ability to achieve their professional and personal duties. Imagine working, studying, and sacrificing for four years that culminates into one final moment before you graduate. Then finding out that you have absolutely no control over it. That’s why the following problem has had the most impact on myself and other students in my class.
Every senior nursing student has to complete a preceptorship in the final semester of their senior year. For this preceptorship, faculty place students on units they feel will promote the development of nursing skills and critical thinking. Nursing students then work on their assigned unit for the entirety of the semester. As the procedure stands now, students have extremely limited knowledge of the process and procedure of preceptor placement. Students also are unable to significantly contribute or express their desires for this last stretch. This has led in my personal experience, and the experiences of others, to substantial stress and anxiety. Currently, the process begins with nursing students filling out a survey depicting their top 3 units they would like to work on during the Spring semester (View Survey below). The College of Nursing faculty and staff then review these surveys and assign students to their units and preceptors.
Faculty have stated that job prospects do not depend on preceptorship. While this is true, this final clinical experience sets the foundation and basis for our future nursing career. This can either negatively or positively affect our view as future nurses. In addition, this final clinical experience can have significant impacts on student nurses’ ability to achieve their professional and personal duties. Imagine working, studying, and sacrificing for four years that culminates into one final moment before you graduate. Then finding out that you have absolutely no control over it. That’s why the following problem has had the most impact on myself and other students in my class.
Every senior nursing student has to complete a preceptorship in the final semester of their senior year. For this preceptorship, faculty place students on units they feel will promote the development of nursing skills and critical thinking. Nursing students then work on their assigned unit for the entirety of the semester. As the procedure stands now, students have extremely limited knowledge of the process and procedure of preceptor placement. Students also are unable to significantly contribute or express their desires for this last stretch. This has led in my personal experience, and the experiences of others, to substantial stress and anxiety. Currently, the process begins with nursing students filling out a survey depicting their top 3 units they would like to work on during the Spring semester (View Survey below). The College of Nursing faculty and staff then review these surveys and assign students to their units and preceptors.
It would be remiss of me not to acknowledge the complexity and difficulty associated with placing upwards of 130 nursing students. However, I feel this is an area of the program where improvement can be made to alleviate the burden and stress of both nursing faculty and nursing students. Nurses in many situations hold lives in their hands. Therefore, student nurses’ educational experiences and learning should be of the utmost importance to the program’s faculty and staff as well as the students. It makes sense for programs to evolve and cater to student needs in order to ultimately meet the needs of the profession itself. The policy and procedure change I propose below will make the program stronger as a whole and help produce more effective, better equipped nurses ready for the workforce
Main Problem:
Senior preceptorship lacks significant input from students and there is insufficient communication to prospective preceptors/units leading to late unit assignments.
This large overarching problem has been broken down below into smaller parts to allow for greater understanding.
Sub Problem 1: Specialty units have a very limited number of preceptors and students are unable to adequately express why they deserve a specialty unit.
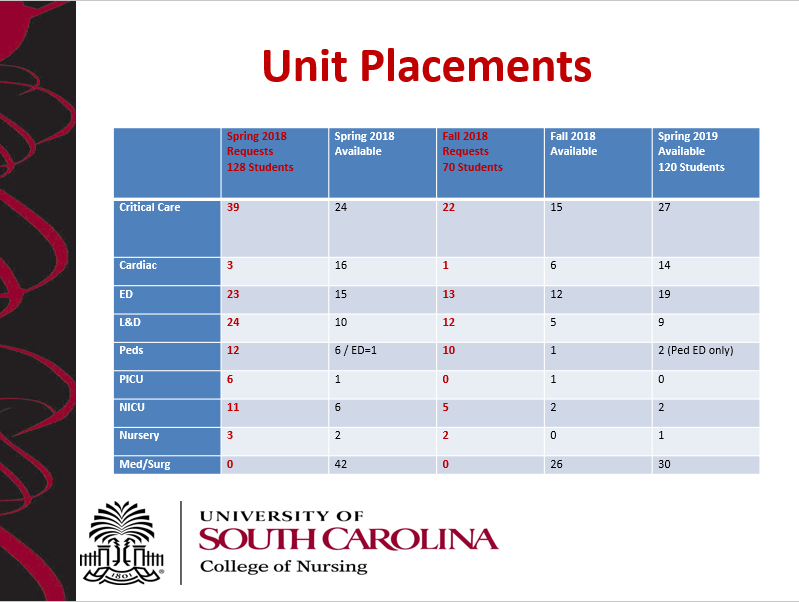
Specialty units such as Pediatrics, Newborn Intensive Care Unit, or the Cardiac Intensive Care Unit are much more difficult to obtain for preceptorship because typically there are only 1-2 preceptors on these units (View preceptor availability below). As you can see based on the chart created by the College of Nursing, these preceptorship experiences are highly competitive.
Additionally, in order for students to be eligible for a specialty unit, they must be endorsed by a previous clinical instructor. However, students are not allowed to ask for a clinical instructor’s endorsement. This begs the question “If students are not allowed to ask clinical instructors to endorse them for a particular unit. How are clinical faculty supposed to know which specialty students desire?”. This inherently places students at a disadvantage. I do agree with this rule to prevent students from bombarding clinical faculty and instead showing their readiness through their clinical expertise and work ethic. However, the only way our voices are heard is through the online survey that we fill out listing our top 3 units. As you saw from the picture, the survey provides no indication of the why we want that unit, why we think we would fit that unit best, or any other personal student information. This limits the input from students.
Sub Problem 2: Preceptors nor units are notified they will have a student in an adequate time.
This problem became relevant when several of my classmates, including myself, were required to change the preceptor or unit they were assigned because the preceptor had no knowledge that they were precepting. Therefore, the unit nor preceptor was able to plan accordingly. I was told at the end of the fall 2019 semester that I was 1 out of 3 chosen for preceptorship on the pediatric unit. However, less than a month before preceptorship began, I was informed that something had happened to my preceptor and my unit had to be changed. I was then placed on the Labor and Delivery unit. You can imagine based on my background as a pediatric cancer survivor how disheartened I was. Similar situations happened with two of my classmates.
One student had chosen to go to the distance location of Augusta SC. Upon arrival to meet her preceptor, this student was informed there was not a preceptor for her. She communicated this with the College of Nursing. While the College of Nursing did work diligently to find her a preceptor, she almost missed a full week of clinicals because of this inadequate communication. Another student was told that he was given weekend nights. He reached out to his preceptor to inform her that he would be her preceptee. During this conversation, the preceptor informed the student that she only worked weekday nights. He informed the College of Nursing faculty who then worked to change his preceptor in time for him to begin clinicals. This is another example of insufficient communication between the College of Nursing and the Unit/Preceptor.
On the other side of the situation, a nurse without prior knowledge that they are precepting or given the opportunity to agree to precept may be frustrated. This is problematic for students, preceptors, and the units themselves. Moreover, not every nurse is suited to precept a student. If units or preceptors were aware of a student coming to precept and learn; they would be better able to meet the needs of that student. This would permit the student a smoother semester, greater prospect for growth, and more learning opportunities. This produces a well-refined, prepared, and confident nurse. In contrast to a nurse partially burnt out from struggling on a unit ill-equipped to aid them in their growth and development as a future nurse.
One student had chosen to go to the distance location of Augusta SC. Upon arrival to meet her preceptor, this student was informed there was not a preceptor for her. She communicated this with the College of Nursing. While the College of Nursing did work diligently to find her a preceptor, she almost missed a full week of clinicals because of this inadequate communication. Another student was told that he was given weekend nights. He reached out to his preceptor to inform her that he would be her preceptee. During this conversation, the preceptor informed the student that she only worked weekday nights. He informed the College of Nursing faculty who then worked to change his preceptor in time for him to begin clinicals. This is another example of insufficient communication between the College of Nursing and the Unit/Preceptor.
On the other side of the situation, a nurse without prior knowledge that they are precepting or given the opportunity to agree to precept may be frustrated. This is problematic for students, preceptors, and the units themselves. Moreover, not every nurse is suited to precept a student. If units or preceptors were aware of a student coming to precept and learn; they would be better able to meet the needs of that student. This would permit the student a smoother semester, greater prospect for growth, and more learning opportunities. This produces a well-refined, prepared, and confident nurse. In contrast to a nurse partially burnt out from struggling on a unit ill-equipped to aid them in their growth and development as a future nurse.
My proposed solution will address all areas of the overarching problem. It will only be effective and fulfill its purpose by utilizing the 3 Life duties discussed throughout my E-portfolio and the theories described in my Key Insights.
Solution:
Allow students to interview for specialty units
In order to placed on a specialty unit, students would be required to set up an interview on their chosen unit with the unit’s director or charge nurse. However, students would only be permitted to interview on one unit. Students would need to complete this interview before the end of their final Fall semester. This gives the unit and faculty time to decide whether the student is fit for the unit before the beginning of the Spring semester. Students would no longer be required to have a clinical instructor’s endorsement because they would be essentially endorsed by the unit.
The interview would alert units of the possibility of having a student come aboard for a semester. This would then be communicated to preceptors from the unit directors or charge nurse instead of coming from the College of Nursing. This in turn would help ease some the College of Nursing responsibilities. Additionally, unit directors and charge nurses are much more aware of the nurses they have on staff and whether they meet the requirements to be a preceptors. This would expand the number of preceptors the College of Nursing has available to them. In expanding this number, it is possible that specialty unit preceptors will increase addressing the competitiveness of those units. This will certainly aide students in the pursuit of their personal and professional duties.
The interview would be treated as job interview. For some students, this may be the first job interview they have ever had. This provides a lower pressure environment to experiment, learn and improve. It would be an invaluable experience for students to gain insight into the expectations of future employers and how to best prepare for an interview. Additionally, it would promote the student’s ability to succeed in obtaining their ideal job as a nurse.
Through the implementation of my solution, you will see the application of my within the classroom learning and beyond the classroom learning. These applications are directly connected to my Key Insights and help me in the pursuit of Civic duty, Professional duty, and Personal duty. I will apply the theories I have learned in class to promote the advancement of the nursing profession and increase the nursing student program satisfaction. I will utilize the life lessons I have learned from my beyond the classroom experiences to professionally promote and implement change in the College of Nursing BSN program in order to place students in an environment that encourages their growth and development.
The interview would alert units of the possibility of having a student come aboard for a semester. This would then be communicated to preceptors from the unit directors or charge nurse instead of coming from the College of Nursing. This in turn would help ease some the College of Nursing responsibilities. Additionally, unit directors and charge nurses are much more aware of the nurses they have on staff and whether they meet the requirements to be a preceptors. This would expand the number of preceptors the College of Nursing has available to them. In expanding this number, it is possible that specialty unit preceptors will increase addressing the competitiveness of those units. This will certainly aide students in the pursuit of their personal and professional duties.
The interview would be treated as job interview. For some students, this may be the first job interview they have ever had. This provides a lower pressure environment to experiment, learn and improve. It would be an invaluable experience for students to gain insight into the expectations of future employers and how to best prepare for an interview. Additionally, it would promote the student’s ability to succeed in obtaining their ideal job as a nurse.
Through the implementation of my solution, you will see the application of my within the classroom learning and beyond the classroom learning. These applications are directly connected to my Key Insights and help me in the pursuit of Civic duty, Professional duty, and Personal duty. I will apply the theories I have learned in class to promote the advancement of the nursing profession and increase the nursing student program satisfaction. I will utilize the life lessons I have learned from my beyond the classroom experiences to professionally promote and implement change in the College of Nursing BSN program in order to place students in an environment that encourages their growth and development.
Implementation of Solution
Step 1: In order to begin the process of implementing this into the College of Nursing program I would need to conduct a needs assessment. I would do this first on the USC Lancaster campus. This needs assessment would come in the form of a Google Form survey. This survey would determine if students had poor experiences with preceptor placement. It would also determine if students were open to the interview process and would prefer it over the current process.
Step 2: As a member of the College of Nursing Deans Advisory committee, I have the unique ability to present this procedure change to Dean Andrews for approval. The purpose of the Dean’s Advisory committee is to permit open discussion about the nursing program and how the Dean can improve the program, what our needs are, and how they can be met. After proposing this idea and getting the Dean's approval or suggestions, I would utilize her feedback in order to better develop the interview process to meet the needs of all parties involved.
Step 2: As a member of the College of Nursing Deans Advisory committee, I have the unique ability to present this procedure change to Dean Andrews for approval. The purpose of the Dean’s Advisory committee is to permit open discussion about the nursing program and how the Dean can improve the program, what our needs are, and how they can be met. After proposing this idea and getting the Dean's approval or suggestions, I would utilize her feedback in order to better develop the interview process to meet the needs of all parties involved.
Key Insight Connection
This step is the initiation of my Civic Duty to take an active role in policy/procedure change. In addition, while the Interview process would be a new change. This change would be based off of anecdotal evidence and physical evidence from the survey. After instituting the policy, there may need to be a “trial year” where a campus such as USC Lancaster uses the Interview process to determine its effectiveness. If it is proven to be effective it will go into effect across all campuses. This would be a direct example of Evidence Based Practice that I learned about in NURS 212 and NURS 400. This process of implementation would be very similar to the MUSC Lancaster transition to baby friendly care which I was able to take part in through my beyond the classroom evidence based practice deliverable
Step 3: If the Dean agrees to try the interview process. I would then gain approval from the hospitals for students to interview on units.
Step 4: I would start by discussing the interview process with hospitals' Nursing Directors. If the Nursing Director was receptive of the idea I would then attend a meeting with all the unit directors present to explain the process. This would be much easier than going to each individual unit and meeting with each unit director. During this meeting with all the unit directors, I would detail that the interview has to be initiated by the student and explain that it needed to be treated as a real interview. At the conclusion of the interview the unit director could provide feedback to the student and should attempt to secure a preceptor on that unit for the student based on two factors.
However, even if the unit director feels the student is a good fit, it is ultimately the College of Nursing faculty that decides the student’s placement. If the faculty determine that the student is equipped and ready for the specialty unit then the student has a secured an aware preceptor. This ensures that the preceptor and unit have prior knowledge of possibly having a student.
Step 4: I would start by discussing the interview process with hospitals' Nursing Directors. If the Nursing Director was receptive of the idea I would then attend a meeting with all the unit directors present to explain the process. This would be much easier than going to each individual unit and meeting with each unit director. During this meeting with all the unit directors, I would detail that the interview has to be initiated by the student and explain that it needed to be treated as a real interview. At the conclusion of the interview the unit director could provide feedback to the student and should attempt to secure a preceptor on that unit for the student based on two factors.
- If they have a nurse that meets the criteria
- To be Preceptor a nurse must have 2 years’ experience.
- If they feel the student is a good fit on the unit.
However, even if the unit director feels the student is a good fit, it is ultimately the College of Nursing faculty that decides the student’s placement. If the faculty determine that the student is equipped and ready for the specialty unit then the student has a secured an aware preceptor. This ensures that the preceptor and unit have prior knowledge of possibly having a student.
Key Insight Connection
This step in implementing the Interview process helps me work towards achieving my professional duty by advocating for future nursing students to have the best final clinical experience possible in their preceptorship. This would be accomplished by being a Servant Leader, a leadership style I learned about in NURS 428. I would also be sure to utilize my AIDET skills that I Iearned in NURS 312 to communicate with the nursing directors, unit directors, and/or charge nurses. My beyond the classroom experience during my capstone clinicals in NURS 435 on the Labor and Delivery unit taught me to be an advocate for my patients. Over the course of working to implement the Interview process, I would be advocating for a better experience for future nursing students.
Step 5: Debrief the faculty on what their roles in the process are. I would again explain that the interview has to be initiated by the student. The main role they are to take is to communicate with the unit director. If faculty do not feel the student is ready for a specialty unit they would express this to the unit director. A student would be placed on a specialty unit they wanted as long as they were deemed ready, appropriate for the unit, and there was a preceptor available. This communication between unit directors would be no more than what was already expected from faculty at the College of Nursing.
Step 6: Conduct a trial run on the next graduating class to determine if the Interview process is effective and helpful. Based on the finding from the trial run; either permanently implement the Interview process. Or revert to the old process.
Step 6: Conduct a trial run on the next graduating class to determine if the Interview process is effective and helpful. Based on the finding from the trial run; either permanently implement the Interview process. Or revert to the old process.
Key Insight Connection
This final step helps me fulfill my personal duty. I was personally affected and do not feel like my placement pushed me closer towards my Professional nor Personal duty I worked to help future nursing students be in a position to do so. This connects back to my beyond the classroom experience during Denver Day as part of NURS 425. This experience helped me see the real-life application of Piaget and Erikson’s theories of development. While the implementation of the Interview process is the real-life application of Florence Nightingales Metaparadigm theory that I learned about in NURS 212.